Free Fibula Flap Reconstruction
The gold standard for jaw reconstruction after cancer resection, tumour removal, and severe trauma — restoring bone continuity, facial form, and the ability to eat and speak.
What Is Free Fibula Flap Reconstruction?
Free fibula flap reconstruction is a form of microvascular reconstructive surgery in which a segment of the fibula bone (the smaller of the two lower leg bones) is transferred to reconstruct a defect in the jaw. The fibula is harvested along with its dedicated blood vessels — an artery and vein — and these are reconnected to blood vessels in the neck using microsurgical suturing techniques under an operating microscope.
This allows the transferred bone to receive a continuous blood supply in its new location, which is essential for the bone to heal, integrate, and ultimately support function and even dental implants. Without a blood supply, transplanted bone does not survive reliably in the complex environment of the head and neck.
The free fibula flap is the gold standard jaw reconstruction technique and is performed by Dr. Abhisek Chatterjee at Asha Cancer Institute, Rampurhat — bringing microvascular reconstructive capability to patients in Birbhum and surrounding districts who would otherwise need to travel to major metropolitan centres.
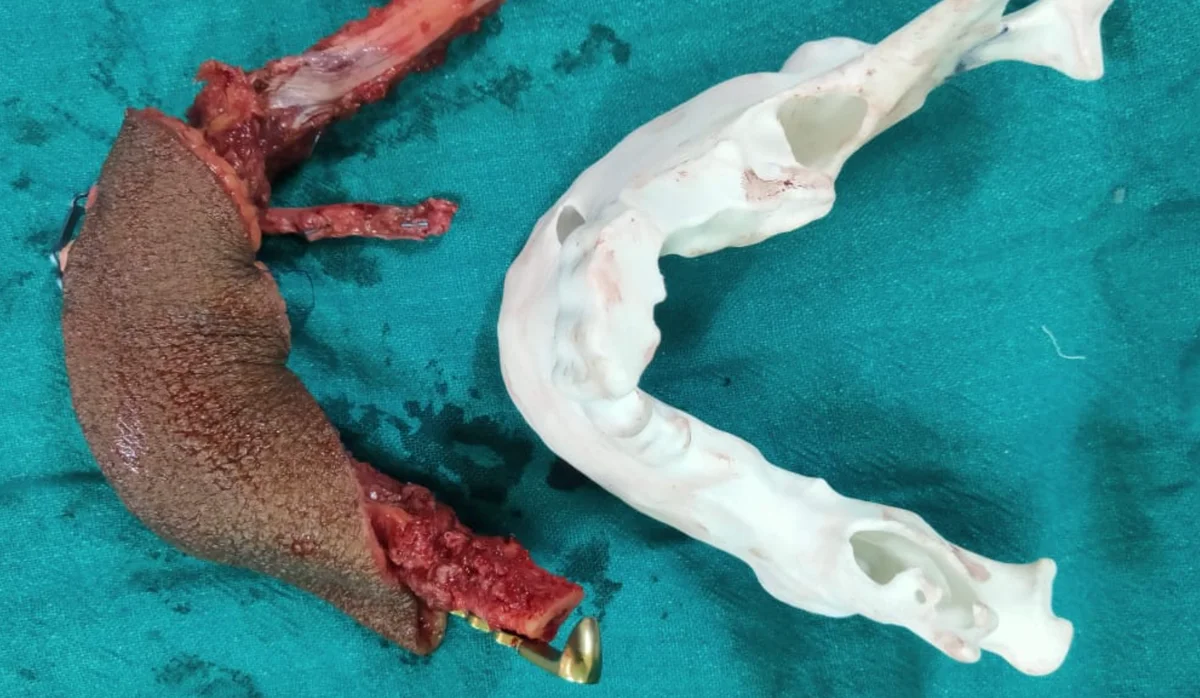
When Is Free Fibula Reconstruction Used?
Jaw Reconstruction After Cancer
The most common indication. When cancer of the jaw (mandible or maxilla) or tongue/floor of mouth with bone invasion requires segmental jaw resection, free fibula reconstruction restores the bone continuity in the same operative sitting.
Jaw Tumour Resection
Wide resection of locally aggressive benign jaw tumours — particularly ameloblastoma requiring segmental mandibulectomy — creates a jaw continuity defect requiring reconstruction with vascularised bone.
Severe Jaw Trauma
Gunshot wounds, road accidents, or blast injuries causing loss of jaw bone and soft tissue may require free fibula reconstruction when the bone defect is too large for simple fixation or conventional bone grafting.
Osteoradionecrosis
Radiation-damaged jaw bone that has undergone necrosis (death) and cannot heal despite conservative treatment may require resection of the necrotic segment followed by free fibula reconstruction.
Why Is the Fibula the Preferred Choice?
The fibula combines multiple characteristics that make it ideally suited for jaw reconstruction — superior to other donor sites for most mandibular defects.
The fibula bone receives a reliable, consistent blood supply from the peroneal artery — making it ideal for free tissue transfer where the blood vessels are disconnected and then reconnected at the new site.
The fibula provides a long segment of bone (up to 22–25 cm) that can be shaped and cut into multiple segments with intervening bone cuts (osteotomies) to recreate the natural curve of the mandible.
A segment of skin and soft tissue (the skin paddle) overlying the fibula can be harvested simultaneously, providing lining tissue to reconstruct the oral mucosa or outer facial skin alongside the bone.
The fibula has sufficient bone height and density to support osseointegrated dental implants — allowing restoration of full dental function months after jaw reconstruction.
The fibula is not the primary weight-bearing bone of the leg (the tibia bears the load). Most patients walk normally within weeks of fibula harvest with appropriate physiotherapy.
How Free Fibula Reconstruction Is Performed
The procedure is carefully planned before the patient enters the operating theatre — making the surgery itself more precise, faster, and predictable.
Planning & Imaging
A CT scan with angiography maps the blood vessels of the leg to confirm a suitable fibula donor site. Virtual surgical planning (VSP) using the patient's CT data allows the jaw reconstruction to be digitally planned — including the size and shape of fibula segments needed, their orientation, and the position of the reconstructed jaw — before surgery begins.
Two-Team Approach
The surgery begins with two simultaneous operative teams. Team one performs the jaw resection (tumour removal or debridement of the damaged jaw). Team two harvests the fibula flap from the lower leg at the same time, reducing overall operating time significantly.
Fibula Shaping
The harvested fibula segment is shaped on the back table. Using custom cutting guides (from pre-operative digital planning), the bone is cut and folded into the correct shape to recreate the jaw curve. Titanium plates are bent and fixed to hold the fibula segments in the planned position.
Jaw Reconstruction
The shaped fibula-plate construct is positioned into the jaw defect and fixed to the remaining native jaw bone with additional titanium screws. The skin paddle is used to reconstruct the oral mucosal lining or skin as required.
Microsurgical Anastomosis
The artery and vein of the fibula flap are connected to blood vessels in the neck using microsurgery — suturing vessels often less than 2–3 mm in diameter under an operating microscope. This step re-establishes blood flow to the transferred bone and tissue.
Monitoring & Healing
The transferred flap is closely monitored in the immediate post-operative period for signs of adequate blood flow. Flap survival rates with experienced microsurgeons are greater than 95%. Healing proceeds over the following weeks as the bone and soft tissue integrate in their new location.
What to Expect: Hospital Stay, Recovery & Eating
Patients are admitted to the surgical ward or intensive care unit for the first 1–2 days for flap monitoring. Nasogastric tube feeding provides nutrition while oral healing begins. Drains from the neck and leg are removed as drainage reduces. Leg physiotherapy begins early to restore normal walking.
Oral feeding progresses from clear fluids to pureed food to soft diet over 4–6 weeks as the surgical wounds heal. Swallowing and speech rehabilitation with a therapist supports recovery of oral function.
The donor leg is initially supported in an elevated position and full weight-bearing is introduced progressively — typically within the first week, guided by the physiotherapist. Most patients return to normal walking within 6–8 weeks. Long-term leg function is generally excellent.
If post-operative histopathology confirms the need for adjuvant radiotherapy or chemoradiotherapy (for oncological cases), this is typically commenced 4–6 weeks after surgery once wounds have healed adequately. The timing is coordinated with the oncology team.
Once the reconstructed jaw has healed, integrated, and recovered from any adjuvant radiotherapy, dental implants can be placed into the fibula bone to restore chewing function. This represents the final stage of jaw rehabilitation — restoring not just the jaw bone but the ability to eat a near-normal diet.
Outcomes & Quality of Life
Free fibula jaw reconstruction significantly improves quality of life after major jaw surgery compared to no reconstruction. Patients who undergo reconstruction are more likely to maintain facial contour, speak intelligibly, eat orally, and reintegrate socially after surgery.
The reconstructed jaw prevents the facial collapse and asymmetry that would result from an unreconstructed jaw defect. Facial form is substantially restored, though some asymmetry may remain.
Speech is typically affected immediately after surgery and improves over months with speech therapy. Most patients achieve intelligible functional speech, though the degree depends on the extent of tongue and soft tissue involvement.
Oral eating is the goal — progressing from liquids to pureed to soft foods over weeks. With dental implants placed into the fibula bone at a later stage, many patients can eat a near-normal diet.
Most patients return to normal walking within 6–8 weeks. Long-term leg function is generally good, with mild ankle and calf changes in a minority of patients.
Why a Specialist Microvascular Surgeon?
Reconnecting blood vessels of 1–3 mm diameter under an operating microscope requires dedicated microsurgical training. Flap survival rates are directly linked to the surgeon's microsurgical experience.
The surgeon performing the resection and the reconstruction must have dual expertise — oncological judgment to achieve clear margins, and reconstructive skill to plan and execute the fibula harvest and inset simultaneously.
Pre-operative digital planning using the patient's CT scan ensures the fibula segments are cut to the precise shape needed to recreate the jaw curve — reducing intraoperative decision-making and operative time.
Microvascular jaw reconstruction has historically been available only at major tertiary centres in Kolkata. Dr. Chatterjee performs this procedure at Asha Cancer Institute, Rampurhat — serving Birbhum and surrounding districts.
Free Fibula Reconstruction FAQs
Need Jaw Reconstruction? Consult a Specialist
Free fibula flap jaw reconstruction is available at Asha Cancer Institute, Rampurhat. Contact Dr. Abhisek Chatterjee for specialist consultation on jaw reconstruction after cancer resection, tumour removal, or trauma.